When my first daughter was born, I was lucky if she slept more than 10 minutes after I put her down. Even placing my daughter in the co-sleeper attached to my bed with my hand on top of her was not successful. Night after night, I held my daughter for hours on my chest. While she slept beautifully, I fought desperately to stay awake out of fear I might harm her. I had heard the warnings regarding bed sharing and certainly didn’t want to do anything to put my baby at risk. Sleep deprivation quickly began to set in. I was dangerously exhausted and in a zombie-like state, too tired to even think straight or enjoy my daughter.
Relief came with a book I was given on infant sleep. It discussed how cultures all over the world sleep with their babies and why and how it can be safe. That night, I followed what my instincts and my daughter were telling me to do. I put my daughter next to me in my bed and we both slept peacefully for the first time ever, waking to nurse and going right back to sleep. At times bed sharing worked beautifully for us and at times it didn’t, but having the option, especially in the early months was a lifesaver!
No sleeping arrangement is 100% safe. Every family is different and bed sharing is not the answer for everyone, yet I strongly believe that parents should be given all the information available on infant sleep in order to make the best decision for their family. Had I been given this information, I would have been able to better enjoy the first weeks of my daughter’s life. The following is an outline of some key information on infant sleep. There are some excellent resources listed also. Please research your options when considering how and where you and your baby will sleep.
“Infants are biologically designed to sense that something dangerous has occurred – separation from the caregiver. They feel, through their skin, that something is different – such as a missing the softness of the mother’s touch, the heat of mother’s body, the smells of mother’s milk, the gentleness of mother’s moving, breathing chest and the feeling of being protected. Infants are alerted because as far as their own body is concerned they are about to be abandoned, and it is therefore time to awaken to call the caregiver back – the very caregiver on whose body the infant’s survival depends.” –James McKenna, Ph.D. Professor of Biological Anthropology, Director, Mother-Baby Sleep Laboratory, University of Notre Dame.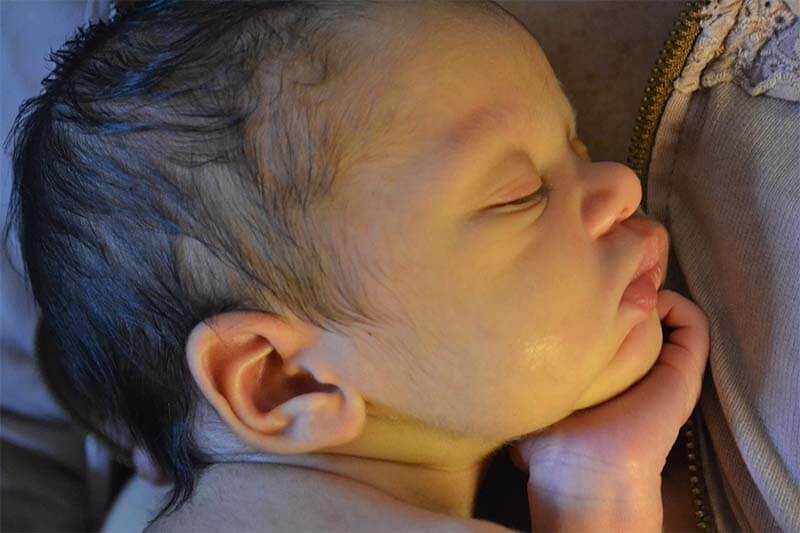
Definitions in research:
Bedsharing- mother and baby sleep on the same surface. This should only include safe sleeping surfaces, not chairs or sofas.
Cosleeping- infant sleeps in proximity (sensory range) of a caregiver, in a crib, bassinet, or co-sleeper attached to the adult bed. This may include bedsharing.
What we know:
- Studies show that 40-80% of parents share sleep with their baby at least some of the time.
- The most common reason parents end up bedsharing is breastfeeding.
- Any breastfeeding for 2-4 months reduces the risk of SIDS by 40%. Any breastfeeding for 6 months or longer reduces the risk by 64%.
- Breastfed babies need to feed at night, often frequently, in order to get enough calories and help the parent make sufficient milk.
- Numerous studies have shown that parents who bedshare breastfeed for longer periods of time than parents who sleep apart from their babies.
- Babies and parents have shared sleep throughout history and in all different cultures.
- When infants and breastfeeding parents are together, their bodies sleep in synchrony. The infant’s wake and sleep cycle, heart rate, breathing, and body temperature are all regulated by the parent’s body. Babies tend to wake more often and sleep more lightly.
- Anti-bedsharing campaigns may be placing breastfed babies at greater risk as parents are falling asleep with their babies on unsafe sleeping surfaces.
- There is not a single study that shows bedsharing is more dangerous than solitary sleep when other risk factors have been accounted for.
- No infant sleeping method is risk-free. It is important for parents to receive all the information they need in order to make the choice that is right for their family. There is not a one-size-fits-all approach to safe infant sleep!
Contributing factors to unsafe sleep:
- Formula feeding
- Someone in the house smokes
- Falling asleep in a chair or sofa
- Alcohol, drug or medications causing fatigue taken by bedsharing parent
- Infant sleeping with someone other than breastfeeding parent
- Prematurity or health issues in the baby
- Overheated baby
- Pillows, blankets, soft beds, cluttered sleeping surfaces
- Babies left alone to sleep or left to cry
- Having other children or pets in the bed
- Stomach sleeping
- Obesity in the bedsharing parent
- Excessive household stress (domestic violence, moving a household, starting daycare)
Safe bedsharing:
- Place baby on back when not breastfeeding
- Sleep on a firm, flat mattress with pillows and heavy blankets away from infant
- Dress infant lightly and make sure he/she is not overheated
- Consider placing mattress on floor or use mesh guardrails, making sure there are no crevices baby can become wedged in
- Infant should only sleep next to the breastfeeding parent
- Never leave baby alone in the bed
- Baby should be full-term and healthy (if not, using a cloth wrap to secure the baby may help stabilize the airway)
- Home should be free of tobacco smoke and the parent should not have smoked during or after pregnancy.
- Extreme fatigue related to a lack of sleep or medications can cause a parent to sleep too deeply, raising the risk of bed sharing.
Further education:
Bedsharing and Breastfeeding: The Academy of Breastfeeding Medicine Protocol #6
BASIS (Baby Sleep Info Source)
Mother-Baby Behavioral Sleep Laboratory at University of Notre Dame, James MCKenna, Ph.D.
Parent-Infant Sleep Lab at Durham University, Helen Ball, Ph.D.
Kathleen Kendall Tackett, Ph.D. IBCLC (research on new mothers and sleep)
Newborns Sleeping Through the Night: A DANGEROUS Myth, Dr. Marcy Axness & Dr. James McKenna
Kangaroo Mother Care: Support for Mothers and Staff of Premature Babies
Skin-to-skin contact requires SAFE TECHNIQUE
Attachment Parenting International, Infant Sleep Safety
AAP Updated 2016 Recommendations for a Safe Infant Sleeping Environment
Nighttime Parenting: How to Get Your Baby and Child to Sleep by William Sears, M.D.
Sleeping with Your Baby: A Parent’s Guide to Cosleeping by James J. McKenna, Ph.D.




Leave A Comment